
New research with MiDOG technology sheds light on the canine oral mycobiome.
Did you know that even if your dog is healthy, they likely have fungal species present in their oral cavity [1]? While fungi are normal components of the canine oral microbiome, in dysbiotic states fungal infections may be associated with the development of periodontitis, an infection that causes inflammation in the oral tissue surrounding and supporting their teeth. Periodontitis is caused by plaque, bacteria, and your dog’s immunologic response to these pathogens, which results in inflammation of the periodontal ligament and alveolar bone [2]. Although the etiology of periodontitis is complex, advancements in diagnostic technology have allowed for an increase in the efficacy of clinical interventions for canines [3].
Our team at MiDOG has collaborated with the Veterinary Dental Specialties and Oral Surgery in San Diego, CA and Veterinary Clinic Arka in Krakow, Poland to produce groundbreaking research characterizing not only the bacteriome of the oral cavity in healthy dogs and dogs with periodontal disease, but also the mycobiome. New research produced from this collaboration is the first of its kind to use Next-Gen Sequencing to investigate the oral cavity of dogs throughout various stages of periodontal disease.

Dr. Brook Niemiec is a Board Certified Specialist in Veterinary Dentistry of both the American and European Veterinary Dental Colleges.
To learn more about the bacteriome of the canine oral cavity, click here.
Periodontitis is painful for your dog and if left untreated can result in serious health complications and even death if the infection does not remain confined to your dog’s mouth. If you suspect your pet has periodontitis, it is recommended that you make an appointment with your veterinarian and determine the diagnostic tools they will be using to improve health outcomes!
Periodontitis Symptoms
As one of the most common oral diseases in canines, periodontitis impacts 44%-100% of canines [2]. Notably, the prevalence and severity of this disease varies significantly based on dog size, breed, and more [2]. Periodontitis manifestation is multifaceted and initially occurs due to a polymicrobial infection caused by oral biofilm, which goes on to trigger an inflammatory immune response. Severe inflammation may lead to the destruction of connective tissue, alveolar bone, and periodontal ligament [4]. Consequently, plaque removal and control are particularly important in preventing periodontitis development [5]. Textured toys and food, daily teeth brushing, and fibrous items that allow the penetration of teeth help decrease the presence of plaque and biofilm [4].
Several studies in recent years have attempted to characterize the mycobial oral profile of healthy and periodontitis impacted canines [6, 7]; however, many of these studies were performed using culture-based methods, “which cannot fully characterize the diversity of the mycobiome due to non-culturables” [7]. Regardless, Malassezia spp and Candida spp were identified at significantly high prevalence rates in different studies [6,7].
When determining the severity of periodontal fungal infection, it is important to assess the virulence factor associated with respective microorganisms; the production of hydrolytic enzymes, proteases and phospholipases, adhesion, formation of germ tube and biofilms should be considered when creating a personalized treatment plan for your dog [6]. It is also important to mention that a variety of factors such as stress, use of broad-spectrum antibiotics or prolonged antibiotic therapy, immunosuppression, age, overcrowding, diets with high carbohydrate concentrations, pH changes, vitamin A deficiencies, preexisting medical conditions, cuts in the oral epithelium, and more can predispose dogs to fungal infections and may increase the likelihood of developing periodontitis [6].
Symptoms to look out for include but are not limited to:
- discolored teeth
- bad breath
- inflammation/bleeding in gums
- loose or missing teeth
- irritability
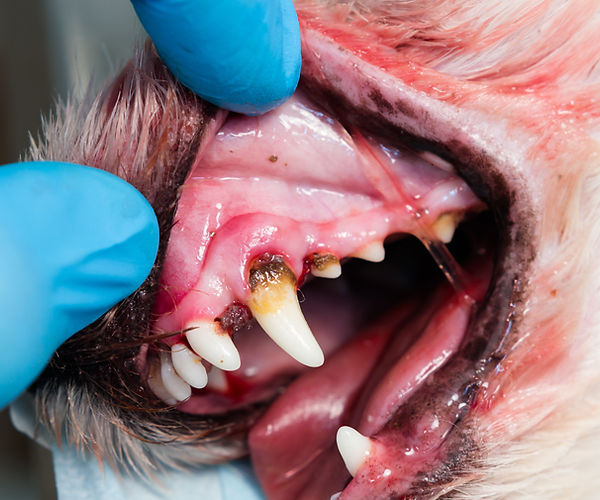
The image above depicts the plaque formation and gum inflammation associated with periodontitis.
Periodontitis Treatment
If a patient is expressing signs of periodontitis, aggressive treatment is required. Once past the first stage (gingivitis) of infection, periodontitis is not easily reversible and extraction may be recommended [5]. Root scaling and planing may also be performed alongside removal of infected/inflamed periodontal tissue [5]. Antibiotics that target the specific foreign bacteria that are causing the infection may be used as well [4]. If you suspect your dog has periodontitis, visit your veterinarian quickly; early intervention can save your dog’s teeth, quality of life, and potentially life.
Advancements in Periodontitis Detection
To determine if a dog is impacted by periodontitis, veterinarians will often perform a conscious, visual exam to take note of the various signs of periodontal disease, such as inflamed gums, plaque build-up, loose teeth, and more [8]. The presence and severity these symptoms may indicate the need for a full work up, in which case the dog is anesthetized and full mouth intra-oral dental radiographs are performed [8]. One study evaluating the validity and reliability of a visual dental scale for detection of periodontal disease in non-anesthetized dogs found that while “an oral examination in an awake dog can be a helpful screening tool, it should not be considered a comprehensive evaluation of periodontal health” [8].
To optimize patient care and accurately identify the specific microbes affecting your dog’s oral health, scientists at MiDOG LLC created a new microbial DNA sequencing-technology that identifies the presence and composition of microbes in patient samples. MiDOG’s sequencing technology has allowed for rapid identification of pathogenic microbes soon after the collection of your pet’s oral sample.
This has revolutionized the ability of veterinary medicine to accurately diagnose and treat canine periodontitis infections. In a collaborative case study led by scientists from MiDOG LLC and researchers from the Veterinary Dental Specialties and Oral Surgery and Veterinary Clinic Arka, the types of fungi present in dogs without periodontal disease, or with mild, moderate, or severe periodontal disease were collected using sterile swabs in the maxillary arcade of each dog. These swabs were then submitted for NGS to compare the mycobiome of the oral cavity in healthy dogs and dogs with various stages of periodontal disease [1].
Establishing the Oral Mycobiome of Clinically Healthy and Periodontitis Impacted Canines
Using MiDOG’s microbial DNA sequencing technology, the oral mycobiome of these canines were established. Notably, fungi were detected in all samples (even clinically healthy ones)! While no single fungal species was found in all samples, the three most frequently found fungal species were Cladosporium sp, Malassezia restricta, and Malassezia arunlokei [1]. Certain fungi, such as those from the Didmellaceae and Irpicaceae family, were significantly associated with different stages of periodontitis [1].
These results are clinically significant, because they highlight that not only are fungi present in the oral cavity of dogs, but there is substantial species diversity with different fungal communities associated with various stages of periodontal disease. NGS provides a uniquely important opportunity for veterinarians to diagnose and treat difficult oral infections.
Read the study here: https://pubmed.ncbi.nlm.nih.gov/34727047/
How Does Your Veterinarian Detect Periodontitis?
The MiDOG All-in-One Microbial Test may provide the answer to the diagnostic conundrum that periodontitis poses. Utilizing NGS technology to detect and quantify all microbial DNA through untargeted and comprehensive sequencing and quantitative comparisons to reference databases, the MiDOG NGS technology provides a useful opportunity to shed light on the microbial makeup of your dog’s oral health for clinical application. The MiDOG microbiome test is a microbial identification test grounded on scientific research that provides veterinarians DNA evidence for the guided treatment of canine infections, such as periodontitis.

Find out if your vet uses MiDOG before you book your next appointment!
Citations:
[1] Niemiec, B. A., Gawor, J., Tang, S., Prem, A., & Krumbeck, J. A. (2021). The mycobiome of the oral cavity in healthy dogs and dogs with periodontal disease. American journal of veterinary research, 83(1), 42–49. https://doi.org/10.2460/ajvr.20.11.0200
[2] Wallis, C. and Holcombe, L., 2020. A review of the frequency and impact of periodontal disease in dogs. Journal of Small Animal Practice, 61(9), pp.529-540.
[3] Bauer, A., Stella, J., Lemmons, M. and Croney, C., 2018. Evaluating the validity and reliability of a visual dental scale for detection of periodontal disease (PD) in non-anesthetized dogs (Canis familiaris). PLOS ONE, 13(9), p.e0203930.
[4] Reiter, A., 2013. Periodontal Disease in Small Animals – Digestive System – MSD Veterinary Manual. [online] MSD Veterinary Manual. Available at: https://www.merckvetmanual.com/digestive-system/dentistry/periodontal-disease-in-small-animals.
[5] Özavci, V., Erbas, G., Parin, U., Yüksel, H. T., & Kirkan, Ş. (2019). Molecular detection of feline and canine periodontal pathogens. Veterinary and animal science, 8, 100069. https://doi.org/10.1016/j.vas.2019.100069
[7] Peters, B. A., Wu, J., Hayes, R. B., & Ahn, J. (2017). The oral fungal mycobiome: characteristics and relation to periodontitis in a pilot study. BMC microbiology, 17(1), 157. https://doi.org/10.1186/s12866-017-1064-9
[8] Zhang, Y., Qi, Y., Lo, E., McGrath, C., Mei, M. L., & Dai, R. (2021). Using next-generation sequencing to detect oral microbiome change following periodontal interventions: A systematic review. Oral diseases, 27(5), 1073–1089. https://doi.org/10.1111/odi.13405
