Rabies is a deadly disease that can impact anyone, not just your furry friends! It is a zoonotic infection, meaning that it is transmitted between animals, and animals can pass it on to humans. World Rabies Day is celebrated to bring awareness to this fatal infection and the importance of staying up to date with pet vaccination records to prevent its spread to you and the pets you care for!
The World Rabies Day 2023 theme is “All for 1, One Health for all” to share the idea that rabies infects more than just the animal population; it infects everyone, including people. The World Health Organization has announced its global goal of “Zero by 30,” which aims to eliminate all dog-mediated human rabies deaths by the year 2030. We all must do our part toward “Zero by 30” and learn more about rabies, its prevention, and its impact on everyone and every pet around us. [1]
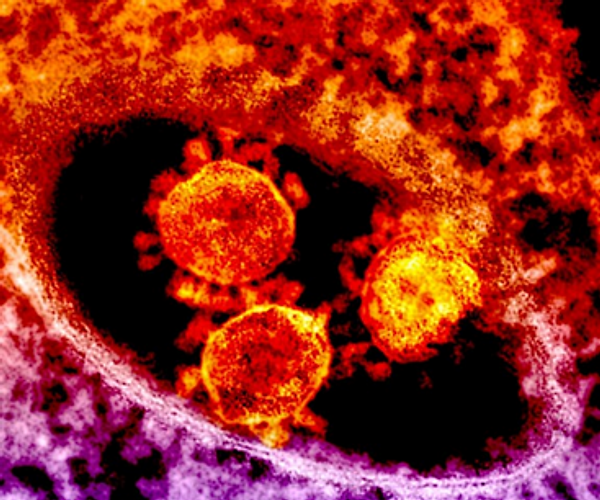
A highly infectious virus, rabies can travel quickly from muscle cells to nerve cells in the brain.
What is rabies?
Rabies is a deadly and highly infectious disease that affects both domestic and wild animals. For World Rabies Day 2023, take the initiative to familiarize yourself with what rabies really is and what it entails for our pets.
Caused by a virus excreted through the saliva of affected animals, the most common transmission of rabies is through bites. The rabies virus cannot pass through intact skin but can pass through cuts, scrapes, bites, or open mouth and nose surfaces. [2]
The incubation period of rabies varies widely. Symptoms could appear within hours or take multiple weeks to appear. Once under the skin, the virus moves from the muscle to nerve cells. From there, the virus will migrate to the brain to begin damaging the nervous system. The virus will attack nerve cells and be excreted in the saliva. [3] If a bite from a rabid animal is to the head, the virus will go directly to the brain, dramatically shortening the incubation period.
What are the symptoms of a rabid pet animal?
Once symptoms begin appearing, stages begin unfolding rapidly. So quickly that a pet can go through all the stages within a week. There are three major stages of rabies in pets:
1. Initial Stage
During the initial stage, pets will begin acting restless and aggressive. Pets could show signs of withdrawal, hiding away and avoiding contact with their family. If the pet is seen licking its bite, it is most likely in the initial stage of infection.
2. Advanced Stage
Aggressive tendencies begin rising to furiousness. The pet could no longer recognize its family and attach their owners. The pet will appear without fear, as if blinded by rage. Dilated pupils and seizures are also common symptoms during the advanced stage.
3. Final Stage
The final stage is characterized by heavy salivating, with the virus now being excreted in the saliva. Pets seem unable to close their mouths, with their jaws slacked constantly. Shortly thereafter, paralysis sets in and eventually leads to coma and death. [3]
How is rabies treated? Can it be prevented?
Once a pet is exposed to rabies, it is almost always fatal. There is no treatment for rabies post-infection. However, rabies is 100% preventable with proper vaccination [4] is so important – to achieve “Zero by 30”, an ambitious goal of taking measures to completely eliminate human death from rabies caused by dog bites by the year 2030.
It is vital to educate pet owners about the seriousness of rabies and the importance of rabies vaccine for dogs, both outdoor and indoor cats, and other pets, especially if there is no evidence of a pet vaccination record for rabies already. You never know when a pet will come into contact with a rabid animal. Vaccinating before an encounter will avoid any unwanted risks and consequences.
How often does your pet dog or cat need the rabies vaccine? Rabies vaccinations are a two-dose process with subsequent boosters. [5] Dogs and cats should receive their first dose at three months and a second dose at twelve months. Boosters should be delivered every three years after the second dose.
Can other pets get rabies besides dogs?
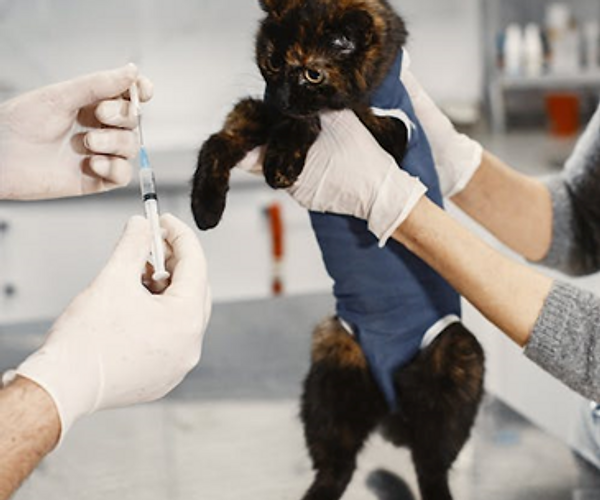
Rabies vaccines should be given at 3 months and 12 months of age, with boosters every three years after.
Another important reason to participate in World Rabies Day 2023 is that the question of “Can _____ get rabies?” is far too common, especially coming from pet owners.
Any mammalian pet is at risk of a rabies infection. Mammalian pets include, but are not limited to, dogs, cats, ferrets, and rabbits. Vaccines are available for dogs, cats, and ferrets. However, there is currently no approved vaccine against rabies for smaller mammalian pets, such as rabbits, guinea pigs, and hamsters. [6]
Can a bird get rabies?
No, reptiles and birds cannot be infected with the rabies virus, so therefore, do not need to be vaccinated. [7]
However, birds and reptiles have their own list of common infections, such as avian candidiasis and respiratory infection in reptiles. If you are someone who either owns or sees these animals as patients, familiarity is recommended.
Do indoor cats need rabies shots?
It is encouraged to vaccinate mammalian pets, regardless of whether they spend their time indoors or outdoors. It is unlikely for indoor pets to have contact with a rabid animal; however, it is still possible. Rabid animals act without fear, so it is possible for them to enter a home if a door is left open.
Can a dog get rabies if vaccinated?
It is unlikely, but yes.
Any pet, not just dogs, can still get rabies if vaccinated but vaccinating is a crucial factor to drastically decrease the chances of infection.
If a cat, dog, or ferret is exposed, they should be brought to an animal health professional and revaccinated immediately. The pet must be observed for 45 days, and any potential signs of illness should be evaluated by an animal health professional and reported to the local health department. If the pet begins to show signs that suggest a rabies infection, then the animal should be euthanized by an animal health professional. [8]
Smaller mammals, such as rabbits, guinea pigs, and hamsters, should be euthanized immediately if exposed to rabies. Rabies is a fatal infection without an approved and properly administered vaccine.
What to do when your pet is overdue for a rabies shot and is exposed to rabies.
If your pet dog is overdue for a rabies shot schedule an appointment with your veterinarian as soon as possible. Up-to-date immunization is the best way to prevent rabies infection, and the risk of infection after exposure increases with delayed vaccination.
If the pet has been vaccinated but is overdue for a booster, the pet should be brought to an animal health professional and revaccinated immediately. The pet must be observed for 45 days, and any potential signs of illness should be evaluated by an animal health professional and reported to the local health department. If the pet begins to show signs that suggest a rabies infection, then the animal should be euthanized by an animal health professional. [8]

Make sure that all pets are up to date on their rabies vaccines!
What can you do as a veterinarian to prevent rabies?
1. Ensure all pet vaccination records are up to date.
Double check the patient’s pet vaccination record to ensure that all pets that are able are vaccinated against rabies and up to date on boosters. The rabies vaccine schedule is typically given at three months and twelve months, with boosters every three years after the second vaccine.
2. Advise your clients on proper preventative measures.
Advise pet owners to be vigilant in keeping their pets away from wild animals. Keeping dogs on leashes while outside and closing doors to prevent unwanted visitors can reduce the risk of being exposed to rabies.
3. Keep you and your clients educated.
Educate yourself and your clients about the severity of rabies and the importance of pet vaccination. Vaccinating sooner rather than later can save a pet’s life!
As a veterinarian, World Rabies Day 2023 is a day to annually check in on your rabies knowledge and renew your rabies preventative protocols at your practice.
Want to learn more? Check out these additional resources for more veterinary information on rabies.
Rabies is a reemerging disease in dogs
Average rabies vaccine and booster cost – Understanding their costs can help you communicate more effectively with pet owners.
Rabies can show up differently in every pet. See how rabies can affect cats and rabbits.
Have a patient that may have been exposed to rabies? Learn more about next steps
Other Common Diseases Veterinarians Should Know
Bacterial Dermatosepticemia in Amphibians
References:
[1] World Health Organization. Accessed 27 September 2023. https://www.who.int/news-room/events/detail/2023/09/28/default-calendar/world-rabies-day-2023
[2] Mahadevan, A. et al. (2016). Perspectives in diagnosis and treatment of rabies viral encephalitis: insights from pathogenesis. Neurotherapeutics, 3(13), 477. doi: 10.1007/s13311-016-0452-4.
[3] Yousaf, M. et al. (2012). Rabies molecular virology, diagnosis, prevention and treatment. Virology journal, 9, 50. doi:0.1186/1743-422X-9-50 .
[4] Brunker, K. & Mollentze, N. (2018). Rabies virus. Microbe of the month, 26(10), 886. doi:10.1016/j.tim.2018.07.001 .
[5] State of California Division of Communicable Disease Control. Accessed 27 September 2023. https://www.cdph.ca.gov/Programs/CID/DCDC/CDPH%20Document%20Library/FactsAboutRabiesVaccinationForCompanionAnimals.pdf docx (ca.gov)
[6] PetMD. Accessed 27 September 2023. https://www.petmd.com/rabbit/conditions/neurological/c_rb_rabies
[7] Colorado Department of Public Health & Environment. Accessed 27 September 2023. https://cdphe.colorado.gov/animal-related-diseases/rabies/rabies-in-colorado
[8] Center for Disease Control and Prevention. Accessed 27 September 2023. https://www.cdc.gov/rabies/specific_groups/veterinarians/potential_exposure.html
[9] Bourhy, H. et al. (2010). Rabies, still neglected after 125 years of vaccination. PLoS Negl Trop Dis, 4(11): e839. https://doi.org/10.1371/journal.pntd.0000839
[10] How much is it? Accessed 27 September 2023. https://www.howmuchisit.org/rabies-shot-cost-dog/
[11] PetCareRx. Accessed 27 September 2023. https://www.petcarerx.com/article/how-do-you-treat-rabies-in-your-cat/4284
Categories: Birds/Parrots, Cats, Dogs, Pet Health, Safety and Wellness, Pet Parents, Rabies, Veterinary Best Practices

